What is it?
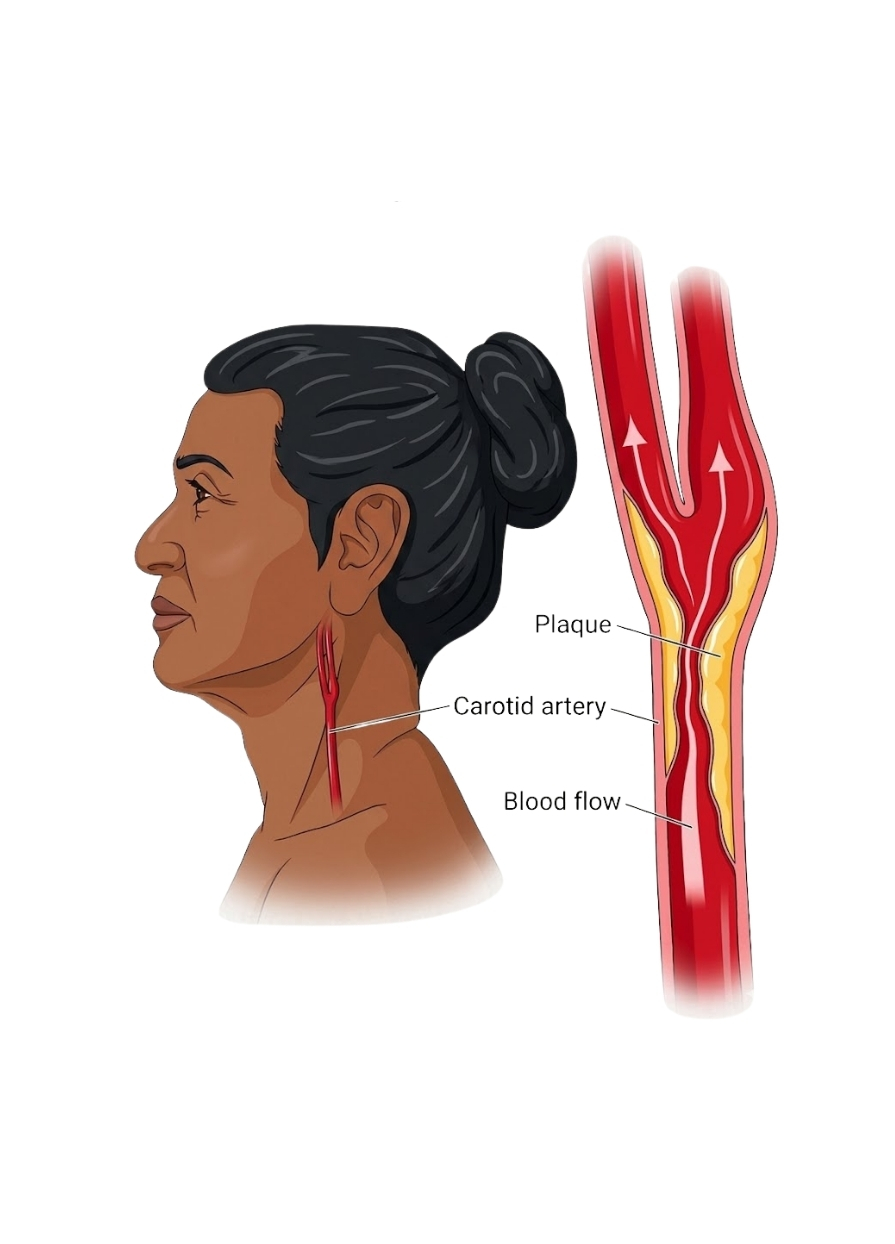
Carotid artery disease, also known as carotid artery stenosis, occurs when the carotid arteries—the vital blood vessels that supply oxygenated blood to your brain—become narrowed or blocked.
This narrowing is caused by the accumulation of plaque, a condition known as atherosclerosis, and significantly increases your risk of having a stroke or a transient ischaemic attack (TIA or ‘mini-stroke’).

Symptoms
In its early stages, carotid artery disease may not produce any signs. Symptoms often only become apparent when the blockage is severe enough to restrict blood flow to the brain, or when a TIA or stroke occurs. Warning signs may include:
- Sudden Numbness or Weakness: Typically affecting one side of the face, an arm, or a leg.
- Speech Problems: Sudden difficulty speaking, slurred speech, or trouble understanding others.
- Vision Issues: Abrupt trouble seeing in one or both eyes, or blurred or darkened vision.
- Dizziness or Loss of Balance: A sudden feeling of dizziness, unsteadiness, or a loss of coordination.
- Severe Headache: A sudden, intense headache with no clear cause.
Causes
Carotid artery disease is most commonly caused by atherosclerosis, the build-up of fatty plaque on the inner walls of the arteries. Factors that contribute to this process include:
- High blood pressure (hypertension)
- High cholesterol
- Diabetes
- Smoking
- Obesity
- Lack of physical activity
- A family history of cardiovascular disease
- Advancing age
Treatments
Dr Shaik offers:
- Carotid Endarterectomy: Surgical removal of plaque from the carotid artery
- Carotid Stenting: Minimally invasive placement of a stent to open the narrowed artery (in selected cases)
- Medical Management: When appropriate, controlling risk factors with medication and lifestyle changes
FAQ
Frequently Asked Questions
The urgency depends on your symptoms and degree of stenosis. If you've had a recent TIA or stroke, surgery may be recommended within days to weeks.
For asymptomatic patients with severe stenosis, surgery can usually be scheduled electively within 4-6 weeks. Your surgeon will assess your individual stroke risk to determine timing.
What are the risks of carotid surgery compared to living with untreated stenosis? Modern carotid surgery carries a stroke risk of 2-3%, whilst severe untreated stenosis carries an annual stroke risk of 5-10% or higher.
Your surgeon will calculate your personalised risk-benefit ratio based on your age, symptoms, degree of stenosis, and other medical conditions to help you make an informed decision.
This depends on the procedure type and your surgeon's preference. Carotid endarterectomy can be performed under general anaesthesia or regional block (where you're awake but the area is numbed).
Some surgeons prefer patients to be awake so they can monitor brain function during the procedure. Carotid stenting is usually performed with conscious sedation.
Regular follow-up with ultrasound scans (typically at 6 months, then annually) helps detect recurrent stenosis. Symptoms to watch for include any return of TIA symptoms, new speech problems, or weakness.
However, recurrence rates are relatively low - less than 10% at 5 years for most patients.
Generally no - bilateral carotid procedures are rarely performed simultaneously due to increased risk. If both arteries need treatment, they're usually staged several weeks apart.
Your surgeon will prioritise which side to treat first based on the degree of stenosis and your symptoms.
Peripheral Arterial Disease
Peripheral arterial disease (PAD) occurs when narrowed arteries reduce blood flow to your limbs, typically the legs. Dr Shaik offers:
- Endovascular Procedures: Minimally invasive techniques including:
- Balloon angioplasty
- Stent placement
- Atherectomy (plaque removal)
- Open Bypass Surgery: Creating alternative routes for blood flow using either synthetic grafts or your own veins when endovascular approaches aren’t suitable
FAQ's
Frequently asked questions
- contact@domain.com
- contact@domain.com

