What is it?
The term ‘diabetic foot’ refers to a range of foot-related complications that commonly affect people with diabetes.
High blood sugar levels over a prolonged period can lead to two main problems that put the feet at risk: nerve damage (peripheral neuropathy) and poor circulation (peripheral arterial disease).
Neuropathy can cause a loss of feeling in the feet, meaning injuries like cuts or blisters may go unnoticed. Poor circulation impairs the body’s ability to heal, so these minor injuries can quickly develop into serious infections, ulcers, and, in severe cases, may require amputation.

Symptoms
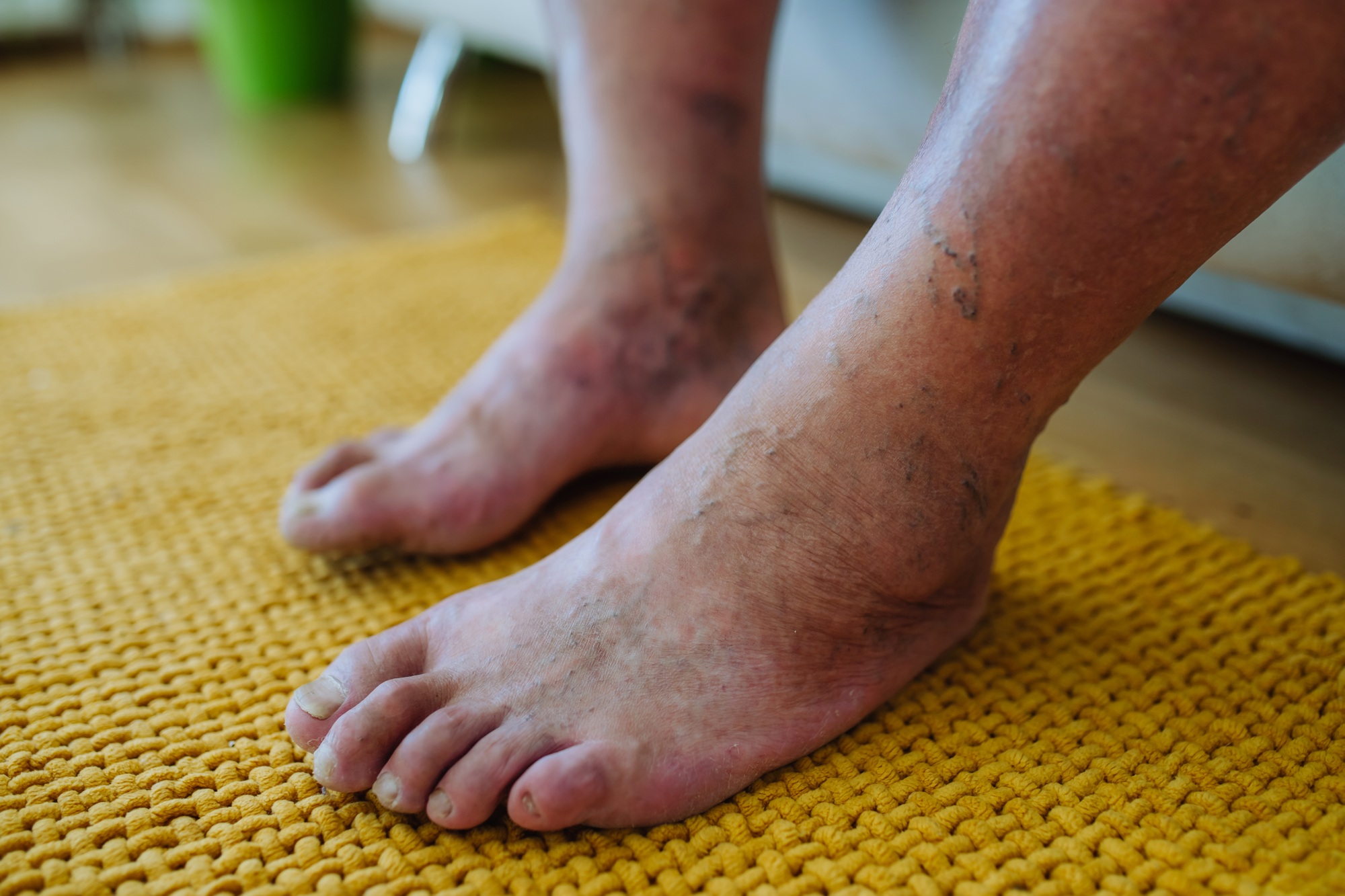
It is vital for individuals with diabetes to inspect their feet daily and be aware of the following signs and symptoms:
- Loss of Sensation: Numbness, tingling, or an inability to feel pain, heat, or cold in the feet.
- Skin Changes: Changes in skin colour or temperature, or skin that is unusually dry, peeling, or cracked.
- Ulcers and Sores: The development of open sores, cuts, or blisters that are slow to heal.
- Pain and Cramping: Aching, cramping, or pain in the calves, thighs, or buttocks during physical activity (claudication).
- Swelling: Unexplained swelling in the feet or ankles.
- Deformities: Changes in the shape of the feet over time, such as hammertoes or Charcot foot.
- Signs of Infection: Redness, warmth, drainage of pus from a wound, or an unpleasant odour.
Causes
The underlying causes of diabetic foot problems are directly linked to the long-term effects of high blood glucose levels (hyperglycaemia):
- Peripheral Neuropathy (Nerve Damage): Sustained high blood sugar can damage the nerves in the feet. This nerve damage reduces sensation, meaning a person may not feel a stone in their shoe, a blister forming, or a small cut. Without this sensory feedback, injuries can worsen without the person being aware of the problem.
- Peripheral Arterial Disease (Poor Circulation): Diabetes accelerates the process of atherosclerosis, where arteries become narrowed and hardened by plaque. This reduces blood flow to the extremities, especially the feet. Good blood circulation is essential for healing, so when it is impaired, even minor injuries can fail to heal properly, leading to the development of chronic ulcers and infections.
- Weakened Immune System: Diabetes can also compromise the immune system, making it harder for the body to fight off infections that may develop in a foot ulcer.
Treatments
Diabetic patients face unique vascular challenges that can threaten limb preservation. Our specialised care includes:
- Wound Debridements: Professional cleaning and removal of non-viable tissue to promote healing
- Pedal Arch Revascularisation: Restoring blood flow to the foot’s arteries to improve healing and prevent amputation
- Comprehensive Care Approach: Collaboration with podiatrists and wound care specialists
FAQ
Frequently Asked Questions
This depends on your risk level. High-risk patients (previous ulcers, severe neuropathy, or poor circulation) may need quarterly visits.
Moderate-risk patients typically need 6-monthly assessments, whilst low-risk patients may only need annual vascular screening. Your team will determine the appropriate frequency for your situation.
Better glucose control is crucial for healing, but existing damage from neuropathy is usually permanent.
However, good control can prevent further nerve damage and significantly improve your body's ability to heal wounds. Most patients see improvement in healing within 2-3 months of achieving better glucose control.
Success rates for diabetic patients are good, though slightly lower than non-diabetics.
Pedal arch revascularisation has success rates of 70-85% for limb salvage. The key is early intervention before extensive tissue loss occurs.
Your surgeon will assess your individual anatomy and likelihood of success.
Home wound care involves cleaning with saline and applying appropriate dressings, but should never involve cutting or aggressive cleaning.
Professional debridement removes dead tissue and biofilm that prevents healing - something that cannot be safely done at home. Attempting to cut away tissue yourself can lead to serious complications.
Seek immediate care for signs of serious infection: red streaking up your leg, fever, chills, rapid spreading of redness, foul-smelling drainage, or if you feel systemically unwell.
Also seek urgent care for any new open wounds, sudden severe pain, or significant colour changes in your foot.
Peripheral Arterial Disease
Peripheral arterial disease (PAD) occurs when narrowed arteries reduce blood flow to your limbs, typically the legs. Dr Shaik offers:
- Endovascular Procedures: Minimally invasive techniques including:
- Balloon angioplasty
- Stent placement
- Atherectomy (plaque removal)
- Open Bypass Surgery: Creating alternative routes for blood flow using either synthetic grafts or your own veins when endovascular approaches aren’t suitable
FAQ's
Frequently asked questions
- contact@domain.com
- contact@domain.com

